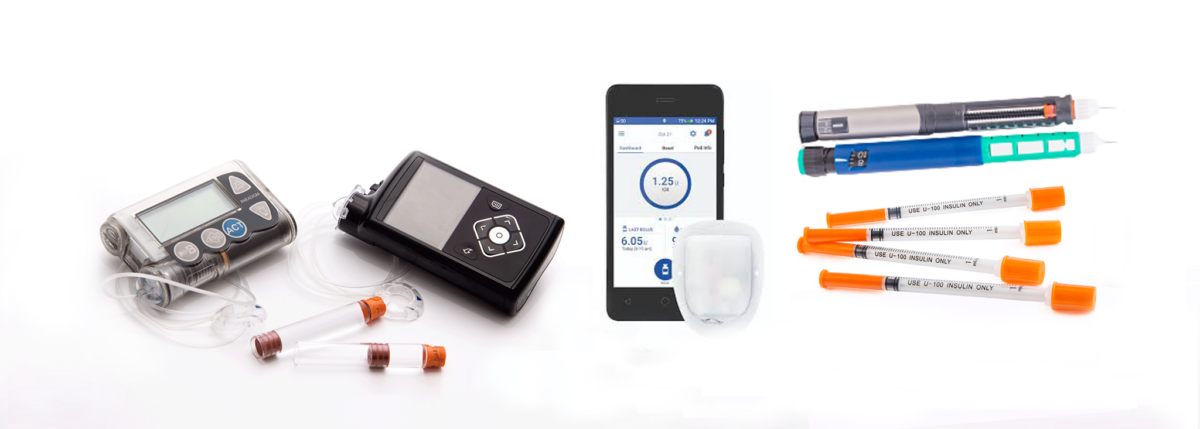
MDI vs Insulin Pumps in Type 2 Diabetes
Depending on one’s health coverage, people with type 2 diabetes (T2D) have a number of choices they can make regarding the management of their condition. Once someone with type 2 diabetes must implement the use of insulin into their everyday life, they have a decision to make regarding how they would prefer to administer that insulin. Typically, there are three available avenues: multiple daily injections (MDI) or insulin pump therapy or insulin “patch” pumps.
Multiple daily injections
MDI is usually the way people with diabetes take insulin. Whether it’s using syringes or pens, insulin injections are taken multiple times per day. They’re taken before meals—to correct for high blood sugar—or to keep blood sugar levels stable throughout the day. MDI has seen its share of technological advances, with the advent of smartpens that are able to automatically log dosages in smartphones and keep the user informed of their total daily insulin usage. However, there are pros and cons to MDI.
Pros:
- Injections are quick and only need to be taken at certain times per day or as needed
- MDI may be beneficial to those who don’t want to be attached to a device
- Simpler to use and easy to learn
- May be less expensive than pump therapy
Cons:
- Injections can be painful and tedious.
- Need to rotate injection sites regularly to improve the effectiveness of insulin delivery
- Higher chance of missing a dose, unless you set a reminder to take insulin or use a smartpen with reminders
- Increased blood sugar variability, especially if you’re taking different types of insulins
Insulin pump therapy
Insulin pumps inject insulin on a continuous basis. The primary benefit of using these devices is the option of adjusting insulin dosages into small increments throughout the day and night, as opposed to one full dose. This precision is useful for those who are seeking ways to fine-tune their blood glucose management. Insulin pumps have been around since the 1970s and have advanced greatly in recent years, with insulin-dependent type 2s now being able to wear insulin pumps such as the tubeless pumps Omnipod System, pictured below. Contrary to what most may believe, people with type 2 diabetes wear insulin pumps instead of primarily relying on injections.
 Pros:
Pros:
- Can receive steady amounts of insulin over time and adjust insulin dosage settings based on your blood glucose patterns. For example, if your blood sugar is higher in the morning than in the afternoon, you can set your insulin pump to give you more insulin in the morning and less in the afternoon.
- Insulin pumps can be worn for two-to-three days at a time.
- Makes carb counting for insulin doses easier. Based on your insulin to carb ratio, your insulin pump can automatically calculate how much insulin you should take based on the number of carbs from your meal.
- Wearing an insulin pump makes it easier to take a correction dose for high blood sugar. Rather than doing the math yourself, manually enter your current blood glucose into your pump device and it will calculate how much insulin you need to get back in range.
- Some pumps can be integrated with continuous glucose monitors (CGMs), allowing pumps to automatically correct high blood sugar.
- Keeps track of how much insulin you’re taking. The extra data from insulin pumps can help you refine your management.
- People with type 2 diabetes can opt for the Omnipod DASH, which is a tubeless pump. This eliminates the chances of pump site rip-off, snagging on other objects, and it adheres to the body anywhere an injection would be given.
- Fewer instances of high and low blood sugars, in other words, it can improve your time-in-range.
Cons:
- Requires training by a certified diabetes educator or an endocrinologist.
- Higher learning curve than using an insulin pen.
- Requires more supplies to use and therefore may be more costly than injections.
- Some users dislike feeling attached to their devices and therefore reminded of their diabetes on a daily basis.
- Insulin pumps may improve blood glucose management, but it won’t solve every blood glucose management issue (i.e. diet, exercise, illness).
- May increase self-consciousness when wearing a pump in intimate situations, social gatherings, formal events, or public places like the beach.
- You may still need to carry an extra pen or syringe to serve a backup for possible pump malfunctions.
- A pump malfunction can increase your risk of diabetic ketoacidosis (DKA).
Disposable insulin “patch” pumps
Disposable insulin “patch” pumps are a newer option for people with type 2 diabetes. Instead of a traditional pump, these patch pumps offer a very simple method of delivering insulin without injections. Determining which type of patch pump is right for you may depend on whether you need both basal (background) and bolus (mealtime) insulin or just bolus insulin.
Pros:
- Set-up and dosing is simple with minimal programming.
- Options include a three-day wearable patch and a one-day wearable patch.
- Options include covering your basal/bolus insulin needs or just bolus insulin needs.
- No additional tech device to carry with you.
- Holds rapid-acting Novolog or Humalog insulin.
- Discrete, thin and comfortable.
- Waterproof for swimming, bathing, etc.
- Does not require batteries.
Cons:
- Requires 24-hour wear.
- Must change daily or every three days depending on the type you choose.
- Like any pump, it can potentially malfunction, requiring you to keep an injection insulin delivery method nearby.
- It must be worn on areas of the body you can easily reach in order to dose insulin at meals.
So what’s right for you?
Injections are cheaper on average as pump supplies can be much more expensive. According to some, there is also a greater risk of developing DKA when using an insulin pump, though many professionals feel this is always preventable if patients are staying on top of their levels.
For some, these reasons are enough to make them stay on MDI. But the advantages of the pump are also important to note. Typically, pump users see fewer sudden highs and lows and the delivery of their insulin is more accurate. The pump allows for more flexibility overall: wearers can go out and seemingly eat what they want because their pump will provide insulin support without them having to think about it. These are all major positives if someone with diabetes doesn’t mind having a permanent reminder of their condition attached to them. However, being on an MDI regimen can mean giving yourself more frequent injections than simply changing your insulin pump site every few days.
Research shows overall, insulin pumps result in better management of blood sugar levels compared to multiple daily injections in people with T2D and even resulted in significant reductions in a patient’s daily insulin requirement as well as a reduction in the frequency and severity of reported hypoglycemic episodes in both type 1 diabetes (T1D) and T2D patients.
When all is said and done, choosing between being on MDI vs. insulin pumps depends solely on you and the lifestyle you wish to lead. Consult a physician’s help and the expertise of a certified diabetes educator, should you want to change the course of your diabetes treatment.